Why Putting A Face To COVID-19 Matters
Identifying the disease is our first step to eliminating its spread.
We can only defeat what we can see.
In order for any nation state to attack the coronavirus epidemic, social distancing and isolation alone are simply not enough. Yes, staying away from the general public helps flatten the curve, but it is identification, data and diagnosis that help stop the spread more than anything.
As of 3/20/20, The United States has tested 80,000 individuals for COVID-19 symptoms. With a population of 350 million, our countries current trajectory is projected to have more cases than any other country in the world.

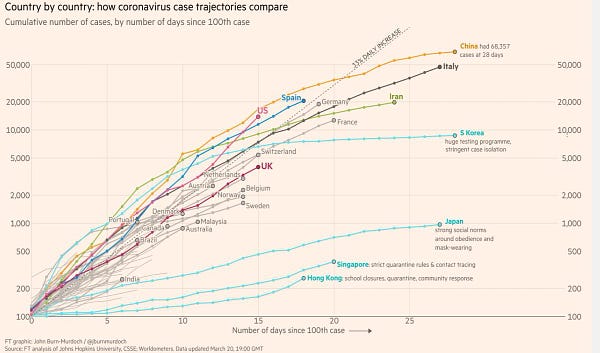
Looking at South Korea on the graph above, they grew cases at a rapid rate, yet were able to diminish future cases thanks to approval from the CDC to test as many individuals as possible. Operating “like an army” according this Reuters report, testing 290,000 people in a seven-week span before the outbreak became widespread.
With a boost in testing, the western world could be able to come up with creative ways to let key businesses open back up and identify low-infected regions of the country to be free for healthy people to go to. A heat map identifying red/green zones, viral regional scores or even determining clearer percentages of a population that are infected.
Come April, small to medium sized businesses will be forced to open their services back up to prevent an even deeper economic recession. With better data insights, we can give regions of the world more peace of mind to operate their natural ways of business and give more resources to regions of the US that need it most.
Below are a few suggestions to help identify the disease:

Tracking Location Data on Social Accounts: There are tools out on the web that can automatically extract data from social media channels, networking sites, blogs, wikis, and news sites. Identifying user-generated content and connecting those posts to the locations that users are associated with. Either tracking content or scrapping profile information.
We will be able to receive an index of locations where people are stating they have the virus or are connected with someone in their network that has causes related to COVID-19. This method is not perfect, as most users of social sites are under the age of 35 and majority of people who contract the virus are over the age of 65… that do not have a digital presence on the web. Not to mention, urban populations are more likely to use digital platforms as compared to rural and potentially impoverished regions who may not have access to digital platforms.
To combat the problems we can have care-takers of older individuals or public service workers in rural populations enter this information manually into a platform or application to represent those folks.
For regions like San Francisco that have a more digitally inclined population, this would be key to ending the lockout for certain blocks and identifying which citizens have the virus to give them more medical attention.
Validating Infected Patient Locations: In the past 10 years we have been lucky to have advancements of technology at our fingertips and at a reasonable price. Being able to scan QR codes for identification, using chips in mobile phones to follow location data and large data storage available to hold the information with cloud technology. Making it possible to find information from people remotely, or at the edge (as technologists have describe the action).
Once a patient is diagnosed at a health care facility, they have the ability to scan a QR code so a governing body can receive insights of where that patient is and where they are connecting locally. This concept has been tried by many organizations over the years, but was tried in a research trial by the National Institutes of Health (NIH) in 2017.
At first glance, it seems a bit “big brother” or a personal privacy concern. Yet in order to comply with Health Insurance Portability and Accountability Act (HIPAA), General Data Protection Regulation (GDPR) and Drug Supply Chain Security Act (DSCSA), we have the ability to anonymize patient information with privacy-preserving technology (Zero-Knowledge Proofs, Federated Learning, Homomorphic Encryption… these topics for another day) to share the health care information with the permissioned parties who need to view that data.
Using this method, we can give rewards to diagnosed patients for staying inside or in a single location over time, giving them an incentive for social isolation and not spreading the virus to more people.

Sensortech Enabled Tracking: Props to Randy Gowat for the original idea. Using Remote thermometers to send to the Center for Disease Control (CDC) or NIH to track potential patients through temperature checking. In this time of a global crisis, most of what hospitals are trying to find out is which patients have similar symptoms or not. Though this typically can be a flawed system because you can have a fever from anything, targeting which patients are ill right now is of most importance.
Online I have found specific remote thermometers prices range anywhere from $75-155 USD on Amazon, Google or on lilsaver.com. We can even get creative in the devices we use to take our temperatures such as a cooking or air quality thermometers which range from $45-100 on Google. This information can be tracked specifically from the device or manually entered in by people to help inform our public health officials of who has a fever. Purchasing of this device should be paid-back by government officials or distributed to households as 1 device/residency.
Obviously obtaining data at the source of the device is better than manually entering it, but it is a solutions that is better than nothing.
Conclusion
These ideas, though bold and require a more digitally inclined population, can be ways to help us put a face to the virus rather than waiting for the infectious disease to go away.
Personally, I would rather us all do something than to just sit on our hands sheltered in place.


